Psoriasis Beta-Blocker Risk Calculator
Risk Assessment Tool
This tool helps you understand your potential risk of psoriasis flare-ups when taking beta-blockers. Based on the information you provide, we'll calculate your personalized risk level.
Your Information
If you have psoriasis and take a beta-blocker for high blood pressure or heart issues, your skin might be reacting in ways you didn’t expect. It’s not just bad luck or stress-it could be the medication itself. Beta-blockers like metoprolol, propranolol, and atenolol are commonly prescribed, but they’re also one of the top drug classes linked to psoriasis flares. Around 20% of people with existing psoriasis see their condition get worse after starting one of these drugs, according to DermNet NZ’s 2022 clinical review. And for some, it’s not just a flare-it’s a full-on outbreak that spreads across the body.
How Beta-Blockers Trigger Psoriasis Flares
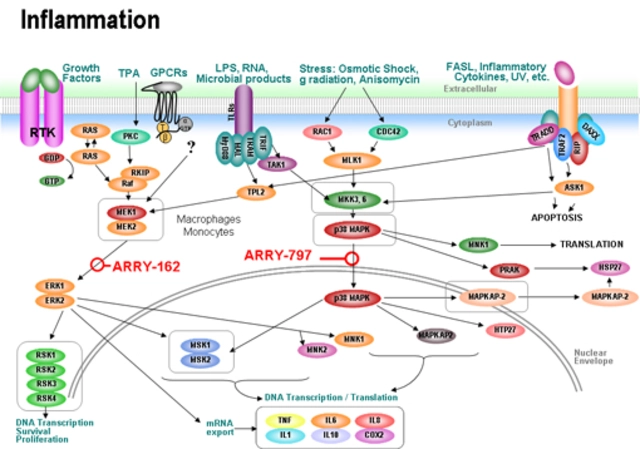
Beta-blockers work by blocking adrenaline from binding to receptors in your heart and blood vessels. That lowers heart rate and blood pressure, which is great for your cardiovascular system. But those same receptors are also found in your skin. When they’re blocked, it messes with how skin cells grow and how your immune system responds.
Here’s what’s happening inside your skin: beta-blockers lower levels of a molecule called cyclic AMP (cAMP). This molecule helps keep skin cell growth in check. When cAMP drops, skin cells multiply too fast-exactly what happens in psoriasis. At the same time, immune cells in the skin get more active, creating inflammation. The result? Thick, red, scaly patches that weren’t there before-or got much worse.
It’s not just any beta-blocker. Propranolol, metoprolol, and bisoprolol are the biggest culprits. Even eye drops like timolol (used for glaucoma) can trigger flares because enough of the drug gets absorbed into your bloodstream through the eye. And it doesn’t happen right away. You might take the drug for months-sometimes up to 18 months-before your skin starts acting up. That delay makes it easy to miss the connection.
Who’s Most at Risk?
Not everyone with psoriasis will react the same way. Some people take beta-blockers for years with no issues. Others see a dramatic worsening within weeks. Research shows that people with a specific gene variant-HLA-C*06:02-are more likely to have a flare triggered by these drugs. This gene is already linked to a higher risk of developing psoriasis in the first place.
Also, if you’ve had psoriasis since your teens or early twenties, you’re more likely to have a reaction than someone who developed it later in life. And if you’ve tried other psoriasis triggers before-like stress, infections, or alcohol-you’re already on higher alert. Adding a beta-blocker into the mix can push you over the edge.
One study from the Journal of the American Academy of Dermatology looked at 110 patients hospitalized for severe psoriasis. Over half of them were taking beta-blockers. The researchers concluded these drugs were a major factor in triggering or worsening their condition. And when they stopped the medication, their skin improved in most cases.
Real Patient Stories
Online forums are full of stories that match the research. On MyPsoriasisTeam, one user wrote: “Started metoprolol for heart palpitations. Six months later, my arms, legs, and scalp were covered in plaques. My dermatologist asked if I’d started any new meds-thank goodness she did.”
Another user on Reddit (r/psoriasis) shared: “I had mild psoriasis on my elbows. After 7 months on propranolol, it exploded. My whole back, chest, even my nails changed. I thought it was stress-turns out it was the beta-blocker.”
These aren’t rare cases. A 2023 survey by MedicalNewsToday found that 37% of psoriasis patients on beta-blockers reported worsening symptoms. Only 12% of those on other blood pressure meds saw the same issue. That’s a big difference.
What to Do If You Suspect a Flare
If you’ve noticed your psoriasis getting worse after starting a beta-blocker, don’t panic-but don’t ignore it either. The first step is to talk to both your cardiologist and dermatologist. This isn’t something you can handle alone. Stopping a beta-blocker without a plan can be dangerous if you have heart disease or high blood pressure.
Your doctors will likely consider switching you to a different type of blood pressure medication. Here are some safer alternatives:
- Calcium channel blockers like amlodipine or diltiazem
- ARBs like losartan or valsartan
- Diuretics like hydrochlorothiazide (in low doses)
Be careful: ACE inhibitors (like lisinopril) can also trigger psoriasis, so they’re not always the best swap. Your doctor will weigh your heart health against your skin health to pick the right one.
In the meantime, your dermatologist may recommend topical treatments-steroid creams, vitamin D ointments, or calcineurin inhibitors-to calm the flare. Light therapy (phototherapy) is also very effective for many people. For severe cases, systemic treatments like methotrexate or biologics might be needed.
Why This Matters More Than You Think
Over 63 million prescriptions for metoprolol were filled in the U.S. in 2023 alone. With about 8.1 million Americans living with psoriasis, there’s a huge overlap. That means tens of thousands of people could be unknowingly worsening their skin condition because of a common heart medication.
The American Heart Association still recommends beta-blockers for many heart conditions-but they now say doctors should consider skin health when choosing treatment. The European Academy of Dermatology even advises dermatologists to ask every patient with new or worsening psoriasis: “Are you on any beta-blockers?”
And here’s the key takeaway: if one beta-blocker triggers your psoriasis, chances are, others will too. Switching from metoprolol to propranolol won’t help. You need to move out of this drug class entirely.

What’s Next? Research and Hope
Scientists are working on better solutions. A 2024 study at Johns Hopkins and Mayo Clinic is looking at genetic markers to predict who’s most at risk. If you carry the HLA-C*06:02 gene, you might be warned before you even start a beta-blocker.
Drug companies are also designing new beta-blockers that target only the heart and not the skin. Early results are promising. In the future, you might get a version that lowers your blood pressure without touching your skin cells.
Until then, awareness is your best tool. If you have psoriasis and take a beta-blocker, keep an eye on your skin. If things change-especially if it’s been 6 to 12 months since you started the med-talk to your doctors. Don’t assume it’s just stress or weather. It might be the medicine.
Quick Summary
- Beta-blockers like metoprolol and propranolol can trigger or worsen psoriasis in about 20% of users.
- Flares can appear 1 to 18 months after starting the drug, making the link hard to spot.
- Stopping the beta-blocker often leads to significant skin improvement.
- Switching to calcium channel blockers or ARBs is usually safer for people with psoriasis.
- If one beta-blocker causes a flare, others likely will too-don’t just switch to a different one in the same class.
Can beta-blockers cause psoriasis for the first time?
Yes, although it’s less common than worsening existing psoriasis. Some people develop psoriasis for the first time after starting a beta-blocker, especially if they have a genetic predisposition. The delay in onset (1-18 months) often makes the connection hard to notice without medical guidance.
Is it safe to stop taking beta-blockers if I think they’re causing my flare?
No-not without talking to your doctor. Beta-blockers are often critical for heart health. Stopping them suddenly can cause rebound high blood pressure, heart palpitations, or even a heart attack. Always work with your cardiologist and dermatologist to find a safer alternative.
What if I need a beta-blocker for my heart condition?
If your heart condition is serious and you absolutely need a beta-blocker, your doctors will work together to manage both conditions. You might use a lower dose, combine it with stronger psoriasis treatments, or use advanced therapies like biologics. In rare cases, newer beta-blockers with less skin impact may be considered in the future.
Are topical beta-blockers (like eye drops) a risk too?
Yes. Even eye drops like timolol can cause psoriasis flares. A small amount gets absorbed into your bloodstream through the eye, and that’s enough to trigger a reaction in sensitive individuals. If you have psoriasis and use glaucoma eye drops, mention it to your dermatologist.
Do all beta-blockers carry the same risk?
No. Propranolol, metoprolol, and bisoprolol have the strongest links to psoriasis flares. Atenolol and pindolol are also known triggers. Newer, more selective beta-blockers may carry lower risk, but there’s still not enough data to say they’re safe. If one triggers a flare, assume others will too.





Emily Wolff
26 February 2026 - 15:09 PM
This is why I stopped taking metoprolol. One month in, my scalp looked like a lava lamp. Dermatologist said, 'You're on a beta-blocker?' Like, duh. Switched to losartan. Skin cleared in weeks. Why isn't this common knowledge?
Jacob Carthy
27 February 2026 - 14:03 PM
Man I had psoriasis since I was 16 and never thought meds could do this. Took propranolol for anxiety and boom full body outbreak. Docs were like oh yeah that happens. Like why dont they tell you this before you take it. Its not like its rare. They just dont care about skin as long as your heart beats
Anil bhardwaj
28 February 2026 - 03:06 AM
I'm from India and my uncle had the same thing. Took atenolol for hypertension, got psoriasis on his hands. He didn't connect it until his dermatologist asked. Now he's on amlodipine and his skin is fine. It's crazy how many people suffer because no one talks about this. Doctors focus on heart and forget skin. Simple fix: ask about meds before treating flare-ups.
lela izzani
1 March 2026 - 13:54 PM
If you're on a beta-blocker and notice your psoriasis changing, don't wait. Go to both your cardiologist and dermatologist together. I did this last year and we switched me from metoprolol to valsartan. The improvement was dramatic within 6 weeks. Topical treatments helped, but removing the trigger was the real win. Also, if you use timolol eye drops for glaucoma - yes, those can do it too. Mention it.
Brandice Valentino
2 March 2026 - 06:22 AM
so i read this article and like wow i didnt know beta blockers could do this. i mean like i have psoriasis and take metoprolol and i thought it was just stress or my diet or something. like why do we even have these drugs if they cause this. its not like theyre new. its been known for years. why is this not on the pill bottle. like come on
Larry Zerpa
3 March 2026 - 00:02 AM
Let me be the one to say it: this isn't a revelation. It's a documented, peer-reviewed, FDA-acknowledged side effect that's been known since the 1980s. The fact that this article treats it like a breakthrough is either dangerously naive or deliberately performative. And the suggestion to 'switch to ARBs'? That's laughable. ARBs have their own psoriasis risks - they're not a magic bullet. You're trading one risk for another. And don't get me started on the 'biologics are the answer' fantasy. They cost $100k a year. This isn't healthcare - it's a profit-driven game of whack-a-mole.
Holley T
3 March 2026 - 14:36 PM
I'm going to be real here - I’ve been living with psoriasis since I was 19, and I’ve been on beta-blockers for over a decade. I started on propranolol for palpitations, then switched to metoprolol because my doctor said it was 'less likely' to cause flares - which is a myth. My skin went from mild elbows to full-body involvement over 14 months. I didn’t connect it because the onset was so slow. I thought it was stress from work, then my divorce, then my cat dying. Turns out it was the medication. I finally asked my dermatologist to check my meds - she nearly fell out of her chair. She said, 'We see this all the time. We just don’t ask.' And now I’m on diltiazem. My skin’s 80% better. But here’s the thing: I wish someone had warned me before I started. I wish the cardiology guidelines had a footnote. I wish pharmacies printed something on the label. This isn’t rare. It’s systemic negligence. And it’s not just me - I’ve seen it in at least six other people in my support group. We’re all just trying to live with a heart condition and not be covered in scales.
Ashley Johnson
4 March 2026 - 20:14 PM
This is all part of the Big Pharma cover-up. Beta-blockers are designed to mess with your immune system. The skin flares? That’s just the beginning. They’re testing how your body reacts to toxins before releasing them. I read a whistleblower report once - the FDA knew about this in the 90s. They buried it. Now they’re pushing ‘new’ beta-blockers? Same chemicals. Different names. They’re not trying to fix it. They’re trying to sell you more expensive creams and biologics. And don’t believe the 'switch to ARBs' nonsense - ARBs are just the next trap. They’re linked to lung fibrosis too. Your heart might be fine, but your lungs? You’re not safe. This is why I only use natural remedies now. Apple cider vinegar, turmeric, and prayer. And I don’t trust doctors anymore.